Table of Contents
Non-invasive Ventilation: Introduction

Non-invasive ventilation (NIV) is a treatment option for persons with respiratory failure that improves oxygenation and decreases carbon dioxide levels without requiring intubation. NIV can be provided in a variety of ways, including BiPAP (bilevel positive airway pressure) and noninvasive positive pressure ventilation (NIPPV), both of which are noninvasive mechanical ventilation. This post will look at the many forms of non-invasive ventilation, their benefits, and how to get non-invasive ventilation at home.
What is Non-invasive Ventilation?
Non-Invasive Ventilation (NIV) is a type of respiratory assistance that provides positive pressure ventilation through a mask or nasal prongs. It is used to enhance respiratory function in patients with various respiratory and non-respiratory diseases. NIV is non-invasive and provides respiratory support without the need for intubation.
Invasive Vs Non-invasive Ventilation
To deliver mechanical ventilation, an invasive ventilation tube is inserted via the patient’s mouth or nose and into the trachea. Invasive ventilation is often utilized in more severe cases of respiratory failure, and it is associated with a higher risk of consequences such as infection and lung injury. Because of the lower risk of problems, non-invasive ventilation is often favored when possible.
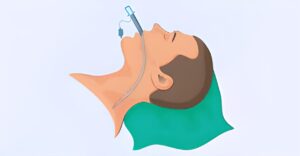
Indications for Non-invasive Ventilation
NIV can be used to manage various respiratory and non-respiratory conditions, including pneumonia, asthma, chronic bronchitis, neuromuscular disorders, cardiogenic pulmonary edema, acute respiratory distress syndrome (ARDS), chronic obstructive pulmonary disease (COPD), heart failure, sleep-disordered breathing
When is NIV Required?
NIV is prescribed for patients who have or are about to have respiratory failure. It can be used as a first-line therapy for individuals experiencing mild to moderate respiratory distress or as a bridge to intubation for patients experiencing severe respiratory distress. Patients with unstable airways, severe hemodynamic instability, or impaired mental status should not receive NIV.
Types of Non-invasive Ventilation
Continuous Positive Airway Airway Pressure (CPAP), Bilevel Positive Airway Pressure (BiPAP), Automated Positive Airway Pressure (APAP), and High-Flow Nasal Cannula (HFNC) are all kinds of NIV. CPAP is used to treat sleep apnea, whilst BiPAP is used to treat respiratory failure or obstructive sleep apnea in patients. APAP titrates the pressure based on the patient’s respiratory pattern, whereas HFNC provides heated, humidified, and high-flow oxygen therapy.
If you are not a medical specialist, the CPAP and BiPAP devices appear similar, but the main difference is the pressure changes when delivering air.
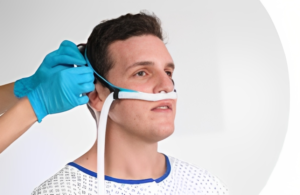
NIV Equipment
A mask or nasal prongs, tubing, and a machine are all part of the NIV equipment. Positive pressure ventilation is delivered via the mask or nasal prongs, while the tubing connects the mask or nasal prongs to the machine. The equipment delivers positive pressure breathing and can be adjusted to the patient’s preferred pressure and mode.

Advantages & Disadvantages of NIV
NIV has several advantages, including avoiding intubation, lowering the risk of ventilator-associated pneumonia, and enhancing patient comfort. The risks of air leakage, skin disintegration, and stomach insufflation are among the drawbacks of NIV.
Patient Selection for NIV
Patient selection for NIV is critical to achieving the greatest results. Respiratory distress, respiratory failure, and the danger of respiratory failure are all criteria for selecting patients for NIV. Consider the patient’s breathing rhythm, comorbidities, and underlying disease before selecting the appropriate NIV mode.
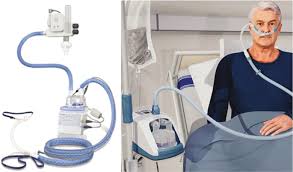
NIV Troubleshooting
Air leakage, skin disintegration, and stomach insufflation are all common complications during NIV treatment. Assessing the patient’s mask fit, altering the pressure settings, and monitoring the patient’s respiratory condition are all steps in troubleshooting.
Conclusion
Non-Invasive Ventilation (NIV) is a useful tool in the treatment of a variety of respiratory and non-respiratory disorders. It allows for positive pressure breathing without the use of intubation, lowers the risk of ventilator-associated pneumonia, and enhances patient comfort.